COVID-19 Spread Slowing In Canada But New Normal Still Far Away
OTTAWA – Life won’t return to the old normal, said Canada’s Chief Public Health Officer Dr. Teresa Tam and her deputy, Dr. Howard Njoo, who presented updated models on COVID-19’s impact in the country Tuesday.
Tam said although the growth of case numbers is slowing, deaths continue to accrue as the virus takes a toll on highly vulnerable populations.
On April 9, when Tam presented an earlier version of the models, the fatality rate was recorded at 2.2 percent. Today, it’s 5.5 percent.
To date, Canada has recorded 49,025 cases and 2,766 deaths from the virus. About 80 percent of those cases are in Ontario and Quebec. The deaths are mostly due to outbreaks in long-term care homes and senior homes. Over 740,500 people have been tested.
The updated models show that by May 5, the country’s cumulative number of cases could reach between 53,196 and 66,835, and deaths could reach between 3,277 and 3,883.
However, Tam says there’s a “leveling off of epidemic trajectories across most jurisdictions in Canada.”
Before public health measures were implemented in March, it was estimated that each infected person transmitted the virus to more than two other people. Today, because of stronger controls, testing, contact tracing, and case isolation efforts, the average number each case infects has been reduced to just above one.
“In order for the epidemic to die out, we need to get to the point where each infected individual is only transmitting the virus to less than one other person,” Tam said.
In addition, the country’s confirmed case count on April 9 was doubling every three-to-five days. That’s now slowed to every 16 days.
“We are making clear progress to slow the spread and bring the epidemic under control thanks to the commitment of Canadians who are following public health advice to protect themselves and others,” she said.
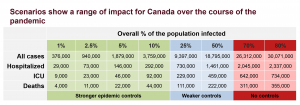
But it’s not time to relax, she says. Public health measures need to be maintained if Canada wants to stay in the current trajectory, which is leading it to a “green zone” of only one-to-10 percent of the population being infected over the course of the pandemic.
“It is critically important that we maintain our public health measures, including physical distancing, until we have achieved epidemic control for the first wave,” she said.
With regional variations, “when and how control measures are readjusted and are relaxed will need to be decided based on the local epidemiological situation,” Tam said.
But any easing of restrictions needs to be done slowly and carefully.
“Each of the provinces and territories, if they’re considering what they might want to do in terms of loosening or relaxing some of the public health measures, you have to ensure you have a good surveillance system, good laboratory capacity, public health system that’s in place to be able to rapidly detect, isolate cases and so on,” said Njoo, adding that they also need to ensure they have the proper hospital capacity.
Public health authorities must be able to dial up measures if there’s a resurgence, he said. Cases need to be detected and managed very quickly, Tam added.
“It’s not that after the first wave we’re in the clear. We’re anticipating a second, third, who knows how many waves,” Njoo said. “But we’re trying to find a manageable level in terms of opening up the economy, and relaxing measures so that people can go outdoors.”
Chief medical officers around the country work together on criteria to help them guide a reopening of the economy and society. But Tam said workplaces need to plan for the new normal. She also said that large gatherings likely happen for a while.
“Until the population has developed a high level of immunity to the virus or we have a vaccine, we have to continue to live with a manageable level of COVID-19 activity,” she said. “Therefore, we anticipate that some public health measures will need to remain in place to prevent the sparking and growth of future epidemic waves.”




